
Treatmentwith NATPAR
NATPAR is indicated as adjunctive treatment of adult patients with chronic hypoparathyroidism who cannot be adequately controlled with standard therapy alone.1
Dosing and titration to achieve the goals of treatment with NATPAR1
Clinical goal: To achieve calcaemic control and to reduce symptoms, while reducing calcium and reducing or discontinuing active vitamin D supplements.
![]()
Please refer to the SmPC for the full dosing and titration section
1. INITIATION
Before initiating NATPAR
- Confirm 25-hydroxyvitamin D stores are sufficient
- Confirm serum magnesium is within range
- Measure serum calcium
Dose initiation table
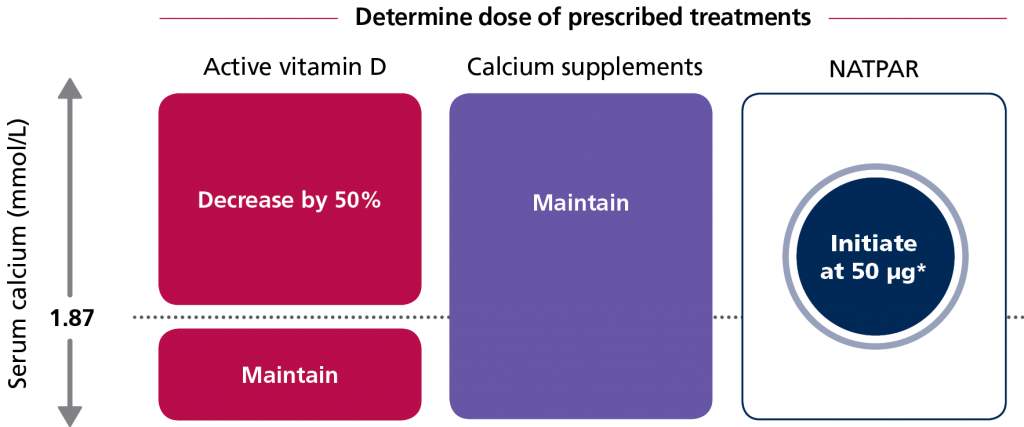
*25 μg can be considered if serum calcium >2.25 mmol/L.

2. DOSE ADJUSTMENT
- Measure pre-dose serum calcium (24 hours after the last injection). Repeat the following day, if it is below 1.87 mmol/L or above 2.55 mmol/L
- Suggested adjustments to active vitamin D and calcium supplements are provided below based on serum calcium value and signs and symptoms of hypocalcaemia or hypercalcaemia

3. TITRATION
- Further adjustment of NATPAR dose can be achieved by measuring post-dose serum calcium levels (8-12 hours after NATPAR injection) following the table below
- Titration timeline is indicative and should be based on clinical assessment. Not all patients may require titration
Dose adjustment table
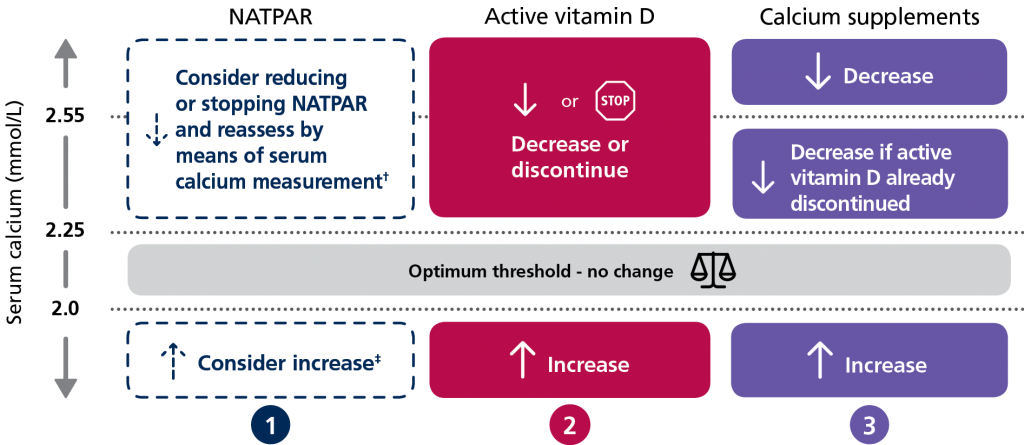
† Downward titration can occur at any time. ‡Dose increments by 25 μg can occur every 2-4 weeks. Measurements of pre and post-dose serum calcium should be repeated and confirmed to be within an acceptable range before titration to a higher dose of NATPAR is considered.
Repeat until clinical goal is met
- Pre-dose serum calcium is between 2.0-2.25 mmol/L
- Active vitamin D has been discontinued
- Calcium supplementation is sufficient to meet daily requirements
NATPAR instructions for use
Click here for full instructions for use
Full instructions on the preparation and injection of NATPAR are provided in the package leaflet. The following video is included as an example of a Takeda resource to support patients taking NATPAR
References
- NATPAR Summary of Product Characteristics.
Natpar® (parathyroid hormone (rDNA)
Detailed Safety Information
Please consult the Natpar Summary Product Characteristics (SmPC) before prescribing.
Natpar treatment should be supervised by a physician or other qualified healthcare professional experienced in the management of patients with hypoparathyroidism. The goal of treatment is to achieve calcaemic control and to reduce symptoms. The optimisation of parameters of calcium phosphate metabolism should be in line with current therapeutic guidelines for the treatment of hypoparathyroidism. Prior to initiating and during treatment with Natpar confirm that 25-OH vitamin D stores are sufficient and that serum magnesium is within the reference range.
Contraindications
Natpar is contraindicated in patients with hypersensitivity to the active substance or to any of the excipients, who are receiving or who have previously received radiation therapy to the skeleton, with skeletal malignancies or bone metastases, who are at increased baseline risk for osteosarcoma, with unexplained elevations of bone-specific alkaline phosphatase, with pseudohypoparathyroidism.
Warnings and Precautions
Monitoring of patients during treatment: pre-dose and in some cases post-dose serum calcium levels must be monitored during treatment with Natpar.
Hypercalcaemia: this was reported in clinical trials with Natpar. Hypercalcaemia commonly occurred during the titration period, during which doses of oral calcium, active vitamin D, and Natpar were being adjusted. Hypercalcaemia may be minimized by following the recommended dosing, the monitoring information and asking patients about any symptoms of hypercalcaemia. If severe hypercalcaemia develops, hydration and temporarily stopping Natpar, calcium and active vitamin D should be considered until serum calcium returns to the normal range. Then consider resuming Natpar, calcium and active vitamin D at lower doses.
Hypocalcaemia: a common clinical manifestation of hypoparathyroidism was reported in clinical trials with Natpar. Most of the hypocalcaemic events occurring in the clinical trials were mild to moderate severity. The risk for serious hypocalcaemia was greatest after the withdrawal of Natpar. Temporary or permanent discontinuation of Natpar must be accompanied by monitoring of serum calcium levels and increase of exogenous calcium and/or vitamin D sources as necessary. Hypocalcaemia may be minimized by following the recommended dosing, the monitoring information, and asking patients about any symptoms of hypocalcaemia.
Concomitant use with cardiac glycosides: Hypercalcaemia of any cause may predispose to digitalis toxicity, monitor serum calcium and cardiac glycoside levels and patients for signs and symptoms of digitalis toxicity.
Severe renal or hepatic disease: Natpar should be used with caution in patients with severe renal or hepatic disease because they have not been evaluated in clinical trials.
Use in young adults: Natpar should be used with caution in young adult patients with open epiphyses.
Tachyphylaxis: the calcium-raising effect of Natpar may diminish over time in some patients. The response of serum calcium concentration to administration of Natpar should be monitored at intervals to detect this and the diagnosis of tachyphylaxis considered.
Urolithiasis: Natpar has not been studied in patients with urolithiasis. Natpar should be used with caution in patients with active or recent urolithiasis because of the potential to exacerbate this condition.
Adverse Reactions
The most commonly observed adverse events with Natpar treatment were hypercalcaemia, hypocalcaemia, headache, diarrhoea, vomiting, paraesthesia, hypoaesthesia and hypercalciuria.
|
Very common
(frequency ≥1/10): |
Hypercalcaemia, hypocalcaemia, headache, hypoaesthesia, paraesthesia, diarrhoea, nausea, vomiting, arthralgia, and muscle spasms. |
|
Common
(≥1/100 to <1/10): |
Hypomagnesaemia, tetany, anxiety, insomnia, somnolence, palpitations, hypertension, cough, upper abdominal pain, muscle twitching, musculoskeletal pain, myalgia, neck pain, pain in extremities, hypercalciuria, pollakiuria, asthenia, chest pain, fatigue, injection site reactions, thirst, anti-PTH antibody positive, blood 25-hydroxycholecalciferol decreased, vitamin D decreased. |
Material code: pi-00658
Date of Preparation of SI: February 2019
Prescribing Information
| Body weight (kg) | Volume to be injected (mL) |
|---|---|
| 38–41 | 0.xx |
| 42–45 | 0.xx |
| 46–49 | 0.xx |
| 50–53 | 0.xx |
| 54–57 | 0.xx |
| 58–61 | 0.xx |
| 62–65 | 0.xx |
| 66–69 | 0.xx |
| 70–73 | 0.xx |
| 74–77 | 0.xx |
| 78–81 | 0.xx |
| 82–85 | 0.xx |
| 86–89 | 0.xx |
| 90–93 | 0.xx |